Understanding the complexities of cardiac arrhythmias is crucial for healthcare professionals, as these conditions can significantly impingement patient health and calibre of life. One such condition is Sinus Exit Block, a type of arrhythmia that affects the heart's natural pacemaker, the sinoatrial node. This status can lead to diverse symptoms and complications, do it crucial for aesculapian practitioners to recognize and care it efficaciously.
What is Sinus Exit Block?
Sinus Exit Block is a type of cardiac arrhythmia characterise by a failure of the electrical impulse to exit the sinoatrial (SA) node, resulting in a pause or delay in the heart's rhythm. This status can be intermittent or lasting and may cause symptoms such as vertigo, fatigue, and even swoon. Understanding the underlying mechanisms and causes of Sinus Exit Block is vital for accurate diagnosis and effective treatment.
Causes of Sinus Exit Block
Several factors can contribute to the development of Sinus Exit Block. These include:
- Age related changes: As people age, the sinoatrial node may become less efficient, stellar to a higher risk of Sinus Exit Block.
- Medications: Certain medications, such as beta blockers, calcium channel blockers, and digoxin, can affect the heart's electrical conductivity and increase the risk of Sinus Exit Block.
- Electrolyte imbalances: Abnormal levels of electrolytes, such as potassium and magnesium, can disrupt the heart's electric action and contribute to Sinus Exit Block.
- Underlying heart conditions: Conditions such as coronary artery disease, heart failure, and cardiomyopathy can affect the sinoatrial node and increase the risk of Sinus Exit Block.
- Inflammatory conditions: Inflammation of the heart tissue, such as in myocarditis or pericarditis, can disrupt the sinoatrial node's use and lead to Sinus Exit Block.
Symptoms of Sinus Exit Block
The symptoms of Sinus Exit Block can vary widely depending on the hardship and frequency of the arrhythmia. Common symptoms include:
- Dizziness or lightheadedness
- Fatigue or failing
- Shortness of breath
- Chest pain or discomfort
- Fainting or near fainting spells
- Palpitations or a feel of a speed heart
In some cases, Sinus Exit Block may not induce any symptoms, and the condition may be discovered incidentally during a routine electrocardiogram (ECG) or other cardiac tests.
Diagnosing Sinus Exit Block
Diagnosing Sinus Exit Block involves a combination of medical history, physical examination, and diagnostic tests. The following steps are typically imply in the diagnostic procedure:
- Medical history: The healthcare supplier will ask about symptoms, aesculapian history, and any medications the patient is guide.
- Physical examination: A physical exam will be performed to assess the heart's rhythm and any signs of underlying heart conditions.
- Electrocardiogram (ECG): An ECG is a non invasive test that records the heart's electrical action. It can help place the characteristic pauses or delays in the heart's rhythm associated with Sinus Exit Block.
- Holter monitor: A Holter reminder is a portable device that records the heart's electric action over a 24 48 hour period. It can facilitate detect intermittent episodes of Sinus Exit Block that may not be trance on a standard ECG.
- Event recorder: An event record-keeper is a small device that the patient can actuate when symptoms occur. It records the heart's electric action at the time of symptoms, providing valuable information for diagnosis.
- Echocardiogram: An echocardiogram uses ultrasound waves to create images of the heart's construction and function. It can aid identify any underlying heart conditions that may be give to Sinus Exit Block.
Note: In some cases, additional tests such as an electrophysiology study may be recommend to further value the heart's electrical conduction scheme.
Treatment Options for Sinus Exit Block
The treatment of Sinus Exit Block depends on the severity of symptoms, the underlying make, and the patient's overall health. Treatment options may include:
- Lifestyle modifications: Adopting a healthy lifestyle, including regular exercise, a balanced diet, and stress management, can aid ameliorate overall heart health and cut the risk of arrhythmias.
- Medications: In some cases, medications such as atropine or isoproterenol may be order to improve the heart's electrical conduction and reduce the frequency of Sinus Exit Block episodes.
- Pacemaker nidation: For patients with severe or diagnostic Sinus Exit Block, a pacesetter may be recommend. A pacesetter is a small device implanted under the skin that sends electrical impulses to the heart to regulate its rhythm.
Types of Sinus Exit Block
Sinus Exit Block can be relegate into different types based on the pattern of the pauses or delays in the heart's rhythm. The main types include:
| Type | Description |
|---|---|
| Type I (Wenckebach) | Characterized by progressive prolongation of the P P interval until a dropped beat occurs, followed by a shorter P P interval. |
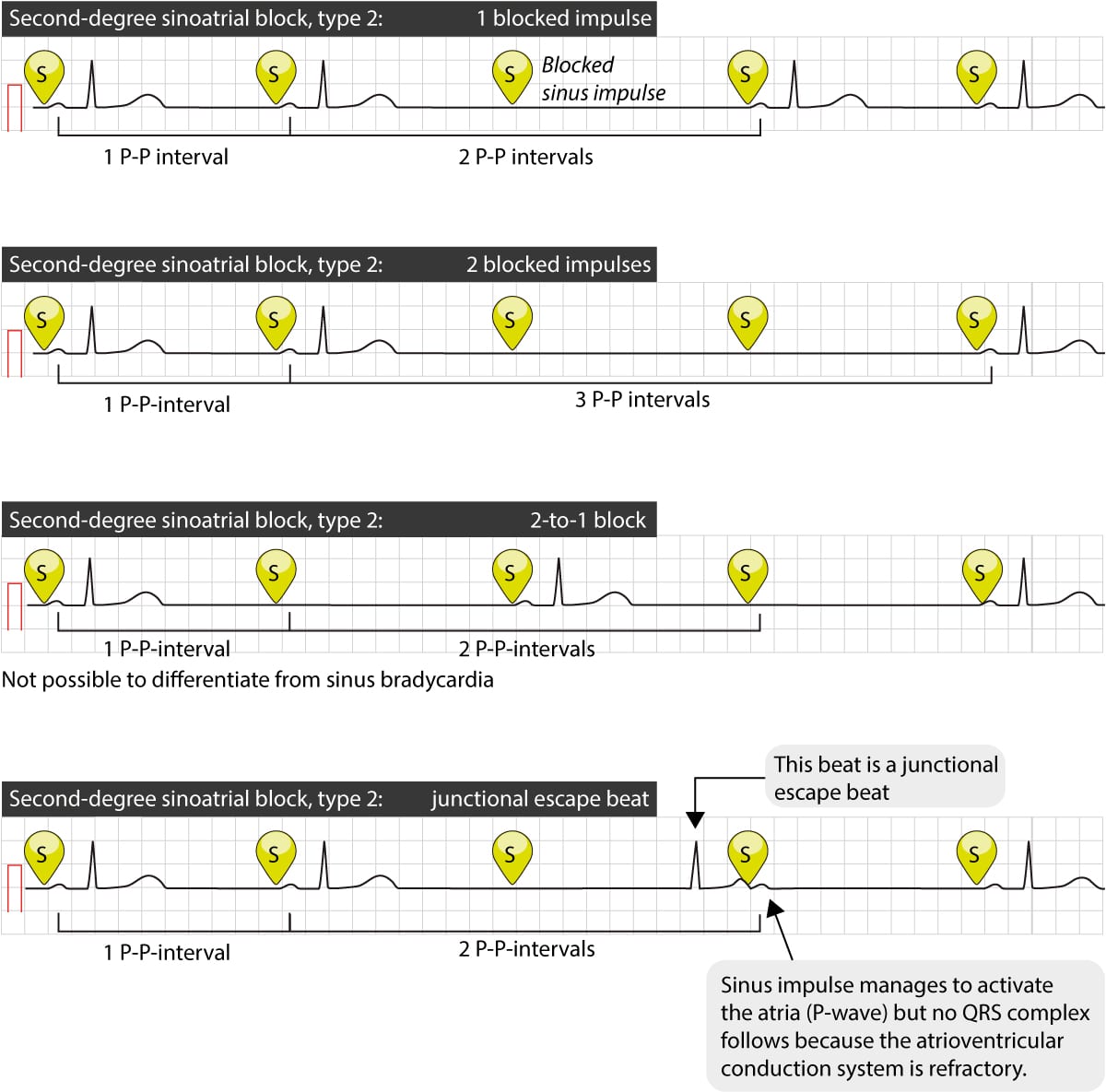
| Type II (Mobitz II) | Characterized by a changeless P P interval with sudden dropped beats. |
| High grade | Characterized by multiple consecutive dropped beats. |
Each type of Sinus Exit Block has its own characteristics and implications for diagnosis and treatment. Accurate designation of the type of Sinus Exit Block is indispensable for efficient management.
Complications of Sinus Exit Block
If left untreated, Sinus Exit Block can result to several complications, include:
- Bradycardia: A slow heart rate can direct to symptoms such as dizziness, fatigue, and fainting.
- Tachycardia: A fast heart rate can occur as a compensatory mechanism, leading to symptoms such as palpitations and shortness of breath.
- Heart failure: Prolonged or severe Sinus Exit Block can contribute to the development of heart failure, a precondition in which the heart is unable to pump blood effectively.
- Stroke: In some cases, Sinus Exit Block can increase the risk of blood clots constitute in the heart, which can travel to the brain and cause a stroke.
Regular monitoring and appropriate treatment can help prevent these complications and amend the patient's caliber of life.
Living with Sinus Exit Block
Living with Sinus Exit Block requires ongoing management and monitoring to ensure optimal heart health. Patients can lead several steps to manage their stipulation effectively:
- Regular follow ups: Regular check ups with a healthcare supplier can help reminder the heart's rhythm and adjust treatment as needed.
- Medication adherence: Taking dictate medications as place can help control symptoms and reduce the risk of complications.
- Lifestyle modifications: Adopting a healthy lifestyle, including regular exercise, a balance diet, and stress management, can improve overall heart health.
- Education: Learning about Sinus Exit Block and its management can help patients better understand their stipulation and conduct an fighting role in their care.
With proper management and indorse, many patients with Sinus Exit Block can take fighting and fulfilling lives.
Sinus Exit Block is a complex condition that requires careful diagnosis and management. By realise the causes, symptoms, and treatment options, healthcare professionals can provide effective care and ameliorate the calibre of life for patients with this condition. Regular monitor, appropriate treatment, and lifestyle modifications are key to managing Sinus Exit Block and preclude complications. With the right approach, patients can lead active and fulfilling lives despite this challenging status.
Related Terms:
- sinus arrest ecg
- sinus arrest
- sinus exit block vs pause
- sinus exit block ecg
- sinus exit block vs arrest
- sinus exit block icd 10